From Classroom to Clinical: Embracing Technology to Prepare Tomorrow’s Nurses
By Sandra Parker
Friday, July 21, 2023

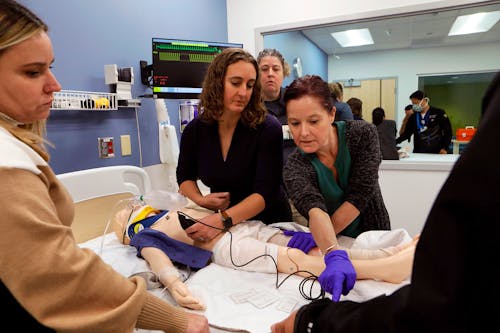
A group of East High School students from the City of Rochester huddle around a mannequin lying on a hospital bed. In a room behind the one-way glass wall, the simulation educator halts our conversation and presses a button on the control panel.
“I’m sore right there,” he says into the microphone.
The words appear to come from the mannequin, causing the students to burst into laughter and jump back from the bed. The students know that real nursing doesn’t involve a talking doll, but it’s a fun way to learn about the field.
The mannequin, a high-tech patient simulator, is one of the technological innovations used by the University of Rochester School of Nursing in transforming its curriculum from the didactic to the interactive and experiential.
The result is graduates who are more competent, confident, and prepared to contribute immediately upon entering the workforce and throughout their nursing careers. The curriculum pivot is vital because lectures are inadequate preparation when searching for a plump vein in the arm of a quivering patient.
However, innovative education is about more than purchasing the latest equipment and using it as directed — the School of Nursing continuously reinvents its curriculum in anticipation of the health care challenges still to come in the 21st century. In recognition of its innovative use of iPads and Apple TV, the School of Nursing has earned Apple Distinguished School status. And judging by the approbation received at a recent conference and requests from other schools for advice, the school is in the vanguard of transforming nursing education.
“We tell potential applicants that if you want to just sit and learn passively through PowerPoints, this isn’t the school for you,” said Erin Baylor, DNP, RN, PNP-BC, ONP, director of simulation.
Message received.
“The technology swayed me into choosing this program,” said Laura-Ann Fierro '23N, who graduated in the spring from the accelerated bachelor’s degree program. “It makes our learning so much easier. I’m as ready as I could ever becoming from nursing school.”
Students practice a wide range of technical, social, and critical skills through simulation with mannequins and standardized patients as well as interactive exercises on the school-issued iPads. For scenarios impractical to reproduce, the school’s virtual technology transports students there. If you have to do it on the job, you can do it here first.
“Thirty years ago, there was no opportunity to safely practice. The first time I inserted a catheter, my hand was shaking,” Baylor said. “Now a student can learn about heart disease and then come in the next day and work on a ‘patient’ with cardiac complaints. It reinforces concepts and translates well to real patients.”
Everyone and everything at the school are linked via an array of the latest software applications. In fact, for most students there is no paper at all except for the diploma. The school-issued student iPad is a curriculum vault, holding textbooks, lectures, interactive clinical exercises, and simulation recordings.
Students have full access anytime to information, which better prepares them for class time that focuses primarily on experiential learning. And no more huddling around the standardized patient being examined; cameras send a live close-up directly to student iPads and to the immense television sets dotting the rooms. The goal is to not only incorporate more technology into the old framework, but to use it to create an entirely new framework.
“We’re officially changing the culture, and now it becomes the norm,” said Tara Serwetnyk, EdD, RN, NPD-BC, director of academic innovation. “We can focus on activities that not only provide practice but foster critical thinking and improve clinical judgment.”
To integrate advanced technology into the curriculum, the school looked to an old Hollywood tactic. Need a hospital? Just make one. And that’s exactly what the School of Nursing did.
Simulation: bringing the clinical setting to the classroom
 To accommodate the school’s reimagined curriculum and technological advancements, three floors were built onto the single-story Helen Wood Hall on Crittenden Boulevard. The $15.1 million expansion added 26,000 square feet and was completed in May 2022. The no-nonsense, brick-and-glass structure is now part hospital, high-tech conference center, classroom, office, and study space. The expansion also allowed ample space for the 169 faculty and nearly 700 students, a 50-percent rise in enrollment since 2016.
To accommodate the school’s reimagined curriculum and technological advancements, three floors were built onto the single-story Helen Wood Hall on Crittenden Boulevard. The $15.1 million expansion added 26,000 square feet and was completed in May 2022. The no-nonsense, brick-and-glass structure is now part hospital, high-tech conference center, classroom, office, and study space. The expansion also allowed ample space for the 169 faculty and nearly 700 students, a 50-percent rise in enrollment since 2016.
Four years earlier, the School of Nursing introduced the iROC initiative to kick off its journey to redefine nursing education. Since then, the curriculum has been radically altered to make it more flexible, efficient, interactive, and relevant to actual clinical practice.
“Today, we live in a world where technology advances at an unprecedented pace, and the profession of nursing is no exception,” said Lydia Rotondo, DNP, RN, CNS, FNAP ,associate dean for education and student affairs and DNP program director.
“As educators, it’s our responsibility to stay on top of technological advancements and find innovative ways to integrate them into our curriculum,” Rotondo added. “By doing so, we provide our students with more personalized and engaging learning experiences, improve access to resources and flexibility, and enhance collaboration and communication among students and faculty. This digital-learning environment enables us to meet learning challenges head on to ensure our graduates have the skills and knowledge needed to succeed in a rapidly changing health-care landscape.”
Nursing education had already moved past the days when students dutifully carried around thick textbooks, listened for hours to anatomy lectures, and occasionally practiced on real patients. But more change was needed to advance deeper into the flipped classroom concept, in which foundational learning is done at home, and class time is free for interactive, collaborative, and critical skill practice. Many nurses working today did few or no simulations in school.
In recognition of the value of simulation, a bill signed by New York Governor Kathy Hochul will allow simulation exercises to count for 30 percent of clinical training hours. Baylor points out that simulation is more varied than clinical training and also more efficient because there is no downtime.
 Simulation training begins in the second week for students in the Accelerated Nursing Programs for Non-Nurses. In one year, students will participate in 15 virtual-reality scenarios and 43 simulations. Students are prepared ahead of time with lecture content, followed by a pre-briefing of the scenario, the simulation, and a debriefing. Some simulations are done with the mannequins, spelled manikins to distinguish them from the non-tech ones common in the fashion industry. The School of Nursing has two SimMan 3G and four SimMan Essential adult manikins. They are high-fidelity, or lifelike, with options for skin tones and gender. Each manikin has a pulse and a port for fluids. Its lungs and intestines make sounds. It can blink, bleed, breathe, and urinate. You can inject it, intubate it, defibrillate it. There is also a baby manikin, a juvenile one that can have a seizure, and a pregnant one that gives birth.
Simulation training begins in the second week for students in the Accelerated Nursing Programs for Non-Nurses. In one year, students will participate in 15 virtual-reality scenarios and 43 simulations. Students are prepared ahead of time with lecture content, followed by a pre-briefing of the scenario, the simulation, and a debriefing. Some simulations are done with the mannequins, spelled manikins to distinguish them from the non-tech ones common in the fashion industry. The School of Nursing has two SimMan 3G and four SimMan Essential adult manikins. They are high-fidelity, or lifelike, with options for skin tones and gender. Each manikin has a pulse and a port for fluids. Its lungs and intestines make sounds. It can blink, bleed, breathe, and urinate. You can inject it, intubate it, defibrillate it. There is also a baby manikin, a juvenile one that can have a seizure, and a pregnant one that gives birth.
Despite these functions, the manikins, of course, still look fake, with their blank stares and perfectly coiffed hair. “We say to the student that we are establishing a fiction contract,” said Kimberly Buholtz, EdD, RN, PED-BC, CHSE, assistant director of simulation. “This might not feel real, but we ask you to treat this as a real patient.”
At first there are a few nervous chuckles, but students quickly become immersed and serious. The simulations are not just about practicing technical skills; students work in pairs to practice collaborating and developing clinical judgment.
“Their actions are very realistic,” said Buholtz. “They’re not treating it as a piece of plastic.”
Students speak to the manikins, who respond, and can also give medications; order and review labs; and call the pharmacy, charge nurse, or the patient’s primary doctor and receive an immediate response. Faculty in the control room are always rooting for the students to make the best decisions. “Sometimes we yell ‘YES!’ and throw our arms up in the air when the students make clinical connections,” Buholtz said.
Students are encouraged to be curious and to explore treatment possibilities. The faculty view it as a psychologically safe place to learn. “They’ll be corrected but not punished for mistakes, which are puzzles to solve,” Buholtz added. “It’s not a gotcha. It’s designed to be a learning experience in a safe way.”
 Joshua Billings '23N, a recent graduate of the accelerated program for non-nurses, said the simulations felt realistic.
Joshua Billings '23N, a recent graduate of the accelerated program for non-nurses, said the simulations felt realistic.
“You’re taking actions as if in a clinical setting, and the effect is weightier than just getting a question answered in class.”
The bulk of the learning takes place in the debriefing room, where students assess the simulation and review the comments made by the faculty member during the session directly onto the video, using SimulationiQ software. Buholtz said she points out the positive actions, not just the areas for improvement.
“A lot of times they’re catching it first. It’s really powerful for them to see it themselves. That’s where the magic is for an educator.”
Recent graduate Fierro found the simulations particularly helpful. “Nursing is not a cookie-cutter profession; there are many different ways to do things,” Fierro said. “A faculty member might ask why we decided to put in a nasal cannula instead of a non-rebreather. And then we can talk about it.”
The simulation videos are saved on the students’ iPads, allowing for later review. In clinical practice, a nurse might not experience a similar scenario for weeks, by which time the particulars aren’t as fresh. With the videos, students can review soon and often, solidifying retention. In addition to providing practice, simulations also present an opportunity for students to take the role of an RN and stretch their skills, which they would not be able to do as a new nurse.
Faculty are constantly retooling and reinventing the scenarios. One in development follows up a clinical simulation with a legal proceeding that centers on the completeness of the nurse’s documentation. The idea is to show the importance of careful notes, which can become part of a lawsuit months or even years later. For situations that are difficult to re-create, there are 10 virtual-reality headsets for a gaming-style, 3D experience of 80 scenarios from Oxford Medical Simulation. With a handheld controller, students participate in the experience by selecting options from a drop-down menu. If it’s a patient visit, they assess the patient, conduct the clinical exam via the nurse avatar, select from a list of questions (the patient answers), order X-rays, read lab reports, and decide on treatment.
The simulation experiences with the manikins and the virtual-reality headset transfer well to the clinical setting, Billings said. “Instead of being worried so much about what I learned step-by-step in class, I’ve done that already, and now I can focus on the patient.”
Billings added that the faculty “did a good job of making it intense enough to mimic but not so intense that it violated that feeling of safety.” The intensity paid off when he had to give CPR to a patient in the hospital. “I felt that I knew exactly what to do because they prepare you well for the high-pressure scenarios.”
The standardized patients also deliver a wide-ranging experience. Some scripts call for shy, confused, or belligerent patients; speakers of languages other than English; and those with a variety of ailments, which can involve wearing a fake bloody wound.
Marlena Gaby-Dater, coordinator of the University of Rochester Standardized Patient Program, said she is impressed with the faculty’s approach to learning. “They don’t just say that the learner’s actions are wrong; they say, ‘These are the things to think about,’” she said. “It’s overall a very supportive environment. You can see that the student is encouraged.”
Gaby-Dater is appreciative of the school’s encouragement of empathy. “They are open to being yourself, and they ask learners what they will do to make patients feel comfortable.”
A focus on innovation and collaboration
 The School of Nursing’s status as an Apple Distinguished School for 2021–2024 makes it one of only five nursing schools across the country to earn the achievement, which recognizes schools that leverage technology to inspire students to learn and empower them to imagine new possibilities.
The School of Nursing’s status as an Apple Distinguished School for 2021–2024 makes it one of only five nursing schools across the country to earn the achievement, which recognizes schools that leverage technology to inspire students to learn and empower them to imagine new possibilities.
Earning the achievement means that technology and digital resources help develop new paths to learning, the faculty are proficient, and the school leadership is focused on continuous innovation.
New students are issued an iPad and immediately trained on its use. In addition to the many standard apps, the school loads several specialty apps that enable students to participate in myriad interactive and collaborative learning activities. There is Panopto for online quizzes, Notability for notetaking, Kahoot! for learning games, AhaSlides for creating presentations, Padlet for sharing information, and VoiceThread for online commenting.
“With the iPad, we can combine didactic and lab and clinical. We’re bringing clinical to the student,” said Kaitlyn Burke, MS, RN, CCRN, CNEcl.
Everywhere you look in the school, there are 70-inch television screens equipped with Apple TV. And with AirDrop, sharing is easy. It takes only a tap on the iPad to show a presentation or an image to everyone in the room. Sharing images comes in handy in the lab and when examining standardized patients. Instead of huddling around the person demonstrating a skill, the view can be shown on the TV so everyone can see and record for later playback.
“Technology can enhance learning,” Serwetnyk said. “It allows us to do less talking at them and more practicing. Students come to class with their pump primed and ready to apply what they’re learning.”
In the lab, students use the iPads to practice electronic documentation. And to coordinate with the day’s skills training, students use Padlet to anonymously share their perspectives on a case study, which facilitates class discussion by drawing in students who might be reluctant to speak up in class. Building competency is more efficient with the many interactive quizzes and other assessments on the iPad, Burke said. So is assessing competency with a tool that shows the number of times students practiced a skill and their level of independence. The school’s preliminary results show that students in the collaborative flipped classroom are more satisfied with the experience and earn higher grades.
Jon Kuppinger, RN, EMT-P, a recent graduate of the RN to BS program, appreciates the fact that everything he needed for the program was loaded on his iPad. As a working nurse, he needed flexibility. “You could do it anytime; I could log on at three in the morning.”
Billings, who has moved to Salt Lake City, said that the constant practice with technology has given him confidence that he can quickly learn whatever technology is used at his new position.
Unlike the isolating role technology played in remote learning during the pandemic, the technology here serves as a unifying force, according to Kuppinger. “It made it a lot more personable. We were able to see each other’s videos and make comments. It keeps you engaged.”
He also found that receiving faculty comments on videos was similar to meeting individually with a professor during office hours and also more convenient.
Fierro, another recent graduate, said it boosted her confidence. “We’re not alone,” she said. Collaboration is a key goal of the program, and the software makes it easy for students to work together to solve clinical problems. So does the arrangement of the tables, which are in groups rather than rows. Redefining nursing education to be more learner-centered means also redefining the role of faculty from lecturer to mentor.
“Nursing is a team sport,” Serwetnyk said. “That’s how you work in the hospital.”
The future of nursing
Factors such as the COVID-19 pandemic and the resulting burnout rate, the nurse shortage, technology changes, and telehealth and other new modes of delivery all disrupted the standard model of nursing education and a nurse’s role in the changing health care environment.
Nurses stand at the intersection of these changes. They will likely be the ones to deliver in-home health care and advocate for health equity and, therefore, need to be aware of the social determinants of health—economic stability, access to quality education and health care, and social and community support.
To prepare nurses to address these emerging priorities, the School of Nursing conducts a poverty simulation that turns students into thespians as they role-play the life of a low-income patient. Sometimes the patient’s car breaks down and they can’t get to work. Sometimes they lose childcare or lose their job. Sometimes racism gets in the way. Ultimately, the patient is forced to choose between buying food or medicine and typically winds up at the pawn shop.
 And with 40 million Americans and nearly half of the City of Rochester’s children living in poverty, the simulation is unflinchingly real. As part of the focus on health equity, nurses need to be aware of health care obstacles so they can advocate for patients who need additional services. Students go into the community to do a windshield survey, in which they videotape and comment on the location and quality of grocery stores, condition of sidewalks, and proximity to transportation. For some students this is an eye-opening experience. It becomes clear that it is not enough to simply advise a patient to take medicine or to exercise or to eat healthy foods. Obstacles can make that advice difficult or even impossible to follow.
And with 40 million Americans and nearly half of the City of Rochester’s children living in poverty, the simulation is unflinchingly real. As part of the focus on health equity, nurses need to be aware of health care obstacles so they can advocate for patients who need additional services. Students go into the community to do a windshield survey, in which they videotape and comment on the location and quality of grocery stores, condition of sidewalks, and proximity to transportation. For some students this is an eye-opening experience. It becomes clear that it is not enough to simply advise a patient to take medicine or to exercise or to eat healthy foods. Obstacles can make that advice difficult or even impossible to follow.
“Nurses need to advocate for patients and understand how social, cultural, and economic factors affect health. They need to assess the patient as a whole person,” Baylor said.
Advances in technology will continue to redefine a nurse’s role. And, as the role evolves, so too does the style and content of nursing education. The goal, according to Baylor, is to use “a student-centered approach with patient-centered outcomes.”
Transforming the curriculum at the School of Nursing better prepares nurses for the workforce and makes education more accessible by offering flexible pathways, such as the 16-month RN to BSN degree being online and an accelerated program offering second bachelor’s degrees in 12 or 24 months. Nine specialties are offered in the master’s programs. It’s not enough to simply adopt technology; it’s also about constantly reinventing and retooling it to, as the saying goes around here, make it ever better. Health care has been disrupted many times before.
Florence Nightingale was a courageous innovator who officially created a new caregiving role—the nurse. In the following decades, however, the contribution of nurses was downplayed; they were referred to as the “physician’s handmaiden.”
A century later, the first dean of the School of Nursing, Loretta Ford, RN, EdD, disrupted health care on a monumental scale by creating another new role—the nurse practitioner. Ford’s views were prescient. She advocated for a healthy lifestyle, health equity, a holistic view of patients, and an expanded role for nurses to deliver quality health care to all communities.
“Nursing must address itself to the health issues of the day,” Ford said in her inaugural address in 1972. “It cannot remain in ivory towers, ignoring the political and social scenes which affect our educational endeavors of practice and our research … Together, we will create a new order of things at the University of Rochester School of Nursing.”
The new order she was creating in the 1960s and beyond wasn’t always welcomed by doctors and others in the medical community. Nevertheless, she persisted.
To Ford, there was no hierarchy in medicine. Just caregivers all.
Today, the School of Nursing embodies Ford’s notion of “a new order of things” as it disrupts the standard nursing education paradigm with one goal in mind: redefining the role of nurses to meet the health care challenges of the 21st century.
Categories: Nursing Education News, Accelerated Programs News